Watch “A Brief Look at Texting and the Internet in Film” from Every Frame a Painting
09 Friday Jun 2023
Posted in Film
≈ Comments Off on Watch “A Brief Look at Texting and the Internet in Film” from Every Frame a Painting
09 Friday Jun 2023
Posted in Film
≈ Comments Off on Watch “A Brief Look at Texting and the Internet in Film” from Every Frame a Painting
07 Wednesday Jun 2023
Posted in Coping Skills
≈ Comments Off on Being Disturbed About Being Disturbed
Isn’t it bad enough to be disturbed about events? Now you find out you can even be disturbed about being disturbed about the event.
A person is so afraid to ride in an elevator, that they develop a phobia about it. Soon, not only anxious about elevators, they worry about anxiety about elevators. “Something is drastically wrong with me,” they think; “Maybe I’m going crazy.” “I should not be so anxious about elevators that I can’t use them; that’s an awful problem; I can’t stand to have this fear; I must certainly be inadequate.” “I know I’m losing control; soon I’ll bet I won’t be able to take care of myself at all; I’ll wind up in a mental hospital.”

Can you see how they are not only fearful of elevators, but down on themselves for being afraid of them? In this case there are two A-B-C sets:
We might find it more efficient to work on the secondary set of A-B-C’s first. Once the person can think differently (more rationally) about having an emotional reaction, they may be more able to concentrate on working through the first set of A-B-C’s.
Do you also have a few sets of secondary A-B-C’s that prevent you from making progress?
05 Monday Jun 2023
Posted in Music
≈ Comments Off on Top Songs I listen to in 2022: SASAMI – Make It Right
04 Sunday Jun 2023
Posted in Data hack, Social Media
≈ Comments Off on Social Leaky Media
Tags
Facebook has been involved in eight data breaches since its launch in 2004. The most famous breach was the Cambridge Analytica scandal, where the company sold the data of 87 million users.
In 2021, Facebook acknowledged a data leak that exposed the personal information of approximately half a billion users. The data included names, birthdays, locations, and phone numbers. Facebook said the leak stemmed from a security problem in 2019 that they had since fixed. They denied any wrongdoing, saying that the data was scraped from publicly available information on the site.
Facebook parent company Meta Platforms agreed to pay $725 million in settlement in a lawsuit seeking damages for allowing third parties, including Cambridge Analytica, access to user data. Facebook users who had an active account at any point between May 2007 and December 2022 can apply to receive a piece of the settlement.

Instagram has had several data breaches in recent years, including:
In August 2020, an unsecured database containing 235 million profiles from Instagram, TikTok, and YouTube was discovered.
In January 2021, a data leak exposed scraped data on 214 million social media accounts.
In September 2022, Irish regulators fined Instagram €405m for data privacy violations.
Instagram was accused of processing children’s privacy data for business accounts and on a user registration platform. Earlier, teen users’ (aged between 13 and 17) accounts were made ‘public’ by default, and they were easily targeted by ads and hacking methods.

Twitter had a data breach in November 2021 that was caused by a vulnerability in Twitter’s software. The vulnerability allowed hackers to learn if an email address or phone number was associated with an existing account. The vulnerability was first flagged to Twitter in January 2022. Twitter fixed the flaw on January 13, 2022.
The breach involved tricking a piece of software linked to Twitter called an API (application programming interface) into revealing hidden details about accounts. Hackers were able to submit an email address or phone number to Twitter’s systems to reveal the username associated with that phone number or email address.
At the end of 2022, there were reports that hackers were selling data stolen from 400 million Twitter users. Researchers now say that a widely circulated trove of email addresses linked to about 200 million users is likely a refined version of the larger trove with duplicate entries removed.
Sources: Wired, Firewall Times, CNN, Verge.
02 Friday Jun 2023
Posted in dogs
≈ Comments Off on Police officer and furry partner share an incredible bond | Pets & Animals | ABC Australia
31 Wednesday May 2023
Posted in Coping Skills, Wellness
≈ Comments Off on Yoga as a practice tool
Today more and more adults practice yoga, and not surprisingly, there is research supporting its physical benefits. Studies show the practice—which combines stretching and other exercises with deep breathing and meditation—can improve overall physical fitness, strength, flexibility and lung capacity, while reducing heart rate, blood pressure and back pain.
But what is perhaps unknown to those who consider yoga just another exercise form is that there is a growing body of research documenting yoga’s psychological benefits. Several recent studies suggest that yoga may help strengthen social attachments, reduce stress and relieve anxiety, depression and insomnia. Researchers are also starting to claim some success in using yoga and yoga-based treatments to help active-duty military and veterans with post-traumatic stress disorder.
“The evidence is showing that yoga really helps change people at every level,” says Stanford University health psychologist and yoga instructor Kelly McGonigal, PhD.
That’s why more clinicians have embraced yoga as a complement to psychotherapy, McGonigal says. They’re encouraging yoga as a tool clients can use outside the therapy office to cope with stress and anxieties, and even heal emotional wounds.
“Talk therapy can be helpful in finding problem-solving strategies and understanding your own strengths and what’s happening to you, but there are times when you just need to kind of get moving and work through the body,” says Melanie Greenberg, PhD, a psychology professor at Alliant International University, who has studied yoga’s benefits to mental health.

The mind-body meld
According to a study by Sherry A. Glied, PhD, professor of health policy and management at Columbia University, and Richard G. Frank, PhD, professor of health-care policy at Harvard Medical School, published in the May/June Health Affairs (Vol. 28, No. 3), the rate of diagnosed cases of mental disorders increased dramatically between 1996 and 2006—doubling among adults age 65 and older, and rising by about 60 percent among adults 18 to 64. During that same time period, rates of psychotropic medication use rose by about the same percentages among these groups.
In light of these numbers, yoga remains a natural and readily available approach to maintaining wellness and treating mental health issues, says Sat Bir Khalsa, PhD, a neuroscientist and professor of medicine at Harvard Medical School at Brigham and Women’s Hospital in Boston who studies yoga’s effects on depression and insomnia. Khalsa, who has practiced yoga for more than 35 years, says several studies in his 2004 comprehensive review of yoga’s use as a therapeutic intervention, published in the Indian Journal of Physiology and Pharmacology (Vol. 48, No. 3), show that yoga targets unmanaged stress, a main component of chronic disorders such as anxiety, depression, obesity, diabetes and insomnia. It does this, he says, by reducing the stress response, which includes the activity of the sympathetic nervous system and the levels of the stress hormone cortisol. The practice enhances resilience and improves mind-body awareness, which can help people adjust their behaviors based on the feelings they’re experiencing in their bodies, according to Khalsa.
While scientists don’t have quite the full picture on how yoga does all that, new research is beginning to shed light on how the practice may influence the brain. In a 2007 study in the Journal of Alternative and Complementary Medicine (Vol. 13, No. 4), researchers at Boston University School of Medicine and McLean Hospital used magnetic resonance imaging to compare levels of the neurotransmitter gamma-aminobutyric acid (GABA) before and after two types of activities: an hour of yoga and an hour of reading a book. The yoga group showed a 27 percent increase in GABA levels, which evidence suggests may counteract anxiety and other psychiatric disorders. GABA levels of the reading group remained unchanged.
“I believe if everyone practiced the techniques of yoga, we would have a preventive aid to a lot of our problems,” Khalsa says. “There would likely be less obesity and Type-II diabetes, and people would be less aggressive, more content and more integrated.”
Khalsa’s claims are backed by evidence supporting the social benefits of participating in a yoga class, says Stanford’s McGonigal. A series of experiments conducted by organizational behavior researchers at Stanford University and published in January’s Psychological Science (Vol. 20, No. 1) suggest that acting in synchrony with others—be it while walking, singing or dancing—can increase cooperation and collectivism among group members.
“In a yoga class, everyone is moving and breathing in at the same time and I think that’s one of the undervalued mechanisms that yoga can really help with: giving people that sense of belonging, of being part of something bigger,” McGonigal says.
Psychologists are also examining the use of yoga with survivors of trauma and finding it may even be more effective than some psychotherapy techniques. In a pilot study at the Trauma Center at the Justice Resource Institute in Brookline, Mass., women with PTSD who took part in eight sessions of a 75-minute Hatha yoga class experienced significantly reduced PTSD symptoms compared with those participating in a dialectical behavior therapy group. The center recently received a grant from the National Center for Complementary and Alternative Medicine to conduct a randomized, single-blind, controlled study to further examine whether, as compared with a 10-week health class, yoga improves the frequency and severity of PTSD symptoms and other somatic complaints as well as social and occupational impairments among female trauma survivors.
“When people experience trauma, they may experience not only a sense of emotional disregulation, but also a feeling of being physically immobilized,” says Ritu Sharma, PhD, project coordinator of the center’s yoga program, who only began practicing yoga when she started leading the program. “Body-oriented techniques such as yoga help them increase awareness of sensations in the body, stay more focused on the present moment and hopefully empower them to take effective actions.”
And in what is becoming one of the most widely applied yoga-based trauma treatments, clinical psychologist Richard Miller, PhD, has developed a nine-week, twice-weekly integrative restoration program based on the ancient practice of yoga Nidra. In 2006, the Department of Defense began testing iRest with active-duty soldiers returning from Iraq and Afghanistan who were experiencing PTSD. At the end of the program, participants reported a reduction in insomnia, depression, anxiety and fear, improved interpersonal relations and an increased sense of control over their lives. Since then, iRest classes have been established at VA facilities in Miami, Chicago and Washington, D.C. Miller has also helped develop similar programs for veterans, homeless people and those with chemical dependencies and chronic pain.
“The program teaches them skills they can integrate into their daily lives, so that in the midst of a difficult circumstance, they have the tools to be able to work in the moment,” says Miller, president of the Integrative Restoration Institute in San Rafael, Calif.
New research is also supporting yoga’s benefit for other mental illnesses. An as-yet-unpublished randomized control trial by Khalsa offers insight into how yoga may reduce insomnia. In this study, 20 participants who practiced a daily 45-minute series of Kundalini yoga techniques shortly before bedtime for eight weeks reported significant reductions in insomnia severity as compared with those told to follow six behavioral recommendations for sleep hygiene. And a 2007 study supports yoga’s potential as a complementary treatment for depressed patients taking antidepressant medication but only in partial remission. University of California, Los Angeles, psychologist David Shapiro, PhD, found that participants who practiced Iyengar yoga three times a week for eight weeks reported significant reductions in depression, anxiety and neurotic symptoms, as well as mood improvements at the end of each class (Evidence-based Complementary and Alternative Medicine, Vol. 4, No. 4). Many of the participants achieved remission and also showed physiological changes, such as heart rate variability, indicative of a greater capacity for emotional regulation, Shapiro says.
Putting yoga into practice
While she cautions against teaching yoga to clients without formal training, McGonigal and others say psychologists can use psychotherapy sessions to practice yoga’s mind-body awareness and breathing techniques. Simple strategies—such as encouraging clients to get as comfortable as possible during their sessions or to pay attention to how their body feels when they inhale and exhale—teach clients to be in the here and now.
“These by themselves would be considered yoga interventions because they direct attention to the breath and help unhook people from thoughts, emotions and impulses that are negative or destructive,” she says.
Alliant International University psychology professor Richard Gevirtz, PhD, agrees that alternatives to traditional psychotherapy may help clinicians make progress with difficult clients.
“Psychologists have painted themselves in the corner by only doing talk therapy,” Gevirtz says. “There’s much more that can be accomplished if you integrate it with other sorts of modalities, such as biofeedback, relaxation training or yoga.”
In fact, some psychologists say yoga may not really be so special when it comes to improving one’s mental state, and that several forms of exercise may provide mood-enhancing benefits.
In a 2007 study by researchers at Bowling Green State University, 36 participants kept mood diaries during the first and final four weeks of a 16-week weight-loss program. On the days participants engaged in planned exercise—typically walking for 30 to 60 minutes—they reported a better mood at night as compared to in the morning, before exercising (Journal of Sport & Exercise Psychology, Vol. 29, No. 6).
“It seems that many types of exercise—particularly non-competitive exercise—are related to positive mood alteration,” says Bonnie Berger, EdD, one of the study’s co-authors and professor and director of Bowling Green’s School of Human Movement, Sport and Leisure Studies.
Psychologists may also benefit from using yoga and other forms of exercise for their own care, Greenberg says. In a 2007 survey of licensed APA members by the APA Board of Professional Affairs Advisory Committee on Colleague Assistance, 48 percent reported that vicarious trauma and compassion fatigue are likely to affect their functioning.
“Practicing yoga personally and adopting a stance based on yoga principles such as non-judgment, compassion, spirituality and the connection of all living things can help relieve stress, enhance compassion and potentially make you a better therapist,” she says. “If you can come to a level of peace with yourself, there may be more nurturing that you exude toward your patients.”
29 Monday May 2023
Posted in TravelTuesday
≈ Comments Off on Saratoga National Cemetery
Tags
Dedicated on July 9, 1999 as Saratoga National Cemetery, it was the 116th National Cemetery. It was renamed to Gerald B. H. Solomon Saratoga National Cemetery on January 24, 2002, in honor of Congressman Gerald B. H. Solomon, who was known for his support of veterans’ causes, and who is interred there. During his tenure in the U.S. House of Representatives, he sponsored the legislation which created the Department of Veterans Affairs and secured approval for the creation of the national cemetery now named for him. He served in Congress from 1979 to 1999, and was Chairman of the powerful Rules Committee in the House at the time of his retirement. As of the end of 2005, only the first 60 acres (240,000 m2) were developed for interments. Gerald B. H. Solomon Saratoga National Cemetery is a United States National Cemetery located in the village of Schuylerville in Saratoga County, New York. Administered by the United States Department of Veterans Affairs, it encompasses 351.7 acres (142.3 ha), and as of 2021 had over 23,000 interments. From Wikipedia.



29 Monday May 2023
Posted in Music
≈ Comments Off on Top Songs I listened to in 2022: MEUTE – Slow Loris
26 Friday May 2023
Posted in Health, Health and wellness
≈ Comments Off on Cleveland Clinic: How to Avoid ‘Tech Neck’ | Andrew Bang, DC
24 Wednesday May 2023
Posted in brain, Depression
≈ Comments Off on Types of Depression
Tags
Whether you’re a college student in the middle of a major slump, a new mom who can’t pinpoint why she’s feeling so glum, or a retiree grieving over the loss of a loved one, that question isn’t an easy one to answer.
But there’s one thing for sure: “It is much more than just a sad mood,” said Angelos Halaris, MD, a professor of psychiatry and medical director of adult psychiatry at the Loyola University Medical Center in Chicago. Symptoms may include everything from hopelessness and fatigue to physical pain. And just as symptoms vary from person to person, so do the actual diagnoses. The word depression is actually just an umbrella term for a number of different forms, from major depression to atypical depression to dysthymia.
The most common form of depression? Major depression. In fact, about 7 percent of the adult U.S. population has this debilitating mental health condition at any given time, according to the National Institute of Mental Health (NIMH).

If you’re experiencing major depression, you may feel and see symptoms of extreme sadness, hopelessness, lack of energy, irritability, trouble concentrating, changes in sleep or eating habits, feelings of guilt, physical pain, and thoughts of death or suicide — and for an official diagnosis, your symptoms must last for more than two weeks. In some instances, a person might only experience one episode of major depression, but the condition tends to recur throughout a person’s life.
The best treatment is usually with antidepressant medications, explained Dr. Halaris, but talk therapy may also be used to treat depression. And there’s good news: An estimated 80 to 90 percent of people with major depression respond well to treatment.
About 2 percent of the American population has a form of depression that’s less severe than major depression but is still very real — dysthymia.
Dysthymia is a type of depression that causes a low mood over a long period of time — perhaps for a year or more, explained Halaris. “People can function adequately, but not optimally.” Symptoms include sadness, trouble concentrating, fatigue, and changes in sleep habits and appetite.
This depression usually responds better to talk therapy than to medications, though some studies suggest that combining medication with talk therapy may lead to the greatest improvement. People with dysthymia may also be at risk for episodes of major depression.
A whopping 85 percent of new moms feel some sadness after their baby is born — but for up to 16 percent of women, that sadness is serious enough to be diagnosable.
Postpartum depression is characterized by feelings of extreme sadness, fatigue, loneliness, hopelessness, suicidal thoughts, fears about hurting the baby, and feelings of disconnect from the child. It can occur anywhere from weeks to months after childbirth, and Halaris explained it most always develops within a year after a woman has given birth.

“It needs prompt and experienced medical care,” he said — and that may include a combination of talk and drug therapy.
Would you prefer to hibernate during the winter than face those cold, dreary days? Do you tend to gain weight, feel blue, and withdraw socially during the season?
You could be one of 4 to 6 percent of people in the United States estimated to have seasonal affective disorder, or SAD. Though many people find themselves in winter funks, SAD is characterized by symptoms of anxiety, increased irritability, daytime fatigue, and weight gain. This form of depression typically occurs in winter climates, likely due to the lessening of natural sunlight. “We don’t really know why some people are more sensitive to this reduction in light,” said Halaris. “But symptoms are usually mild, though they can be severe.”
This depression usually starts in early winter and lifts in the spring, and it can be treated with light therapy or artificial light treatment.
Despite its name, atypical depression is not unusual. In fact, it may be one of the most common types of depression — and some doctors even believe it is underdiagnosed.
“This type of depression is less well understood than major depression,” explained Halaris. Unlike major depression, a common sign of atypical depression is a sense of heaviness in the arms and legs — like a form of paralysis. However, a study published in the Archives of General Psychiatry (now known as JAMA Psychiatry) found that oversleeping and overeating are the two most important symptoms for diagnosing atypical depression. People with the condition may also gain weight, be irritable, and have relationship problems.

Some studies show that talk therapy works well to treat this kind of depression.
Psychosis — a mental state characterized by false beliefs, known as delusions, or false sights or sounds, known as hallucinations — doesn’t typically get associated with depression. But according to the National Alliance on Mental Illness, about 20 percent of people with depression have episodes so severe that they see or hear things that are not there.
“People with this psychotic depression may become catatonic, not speak, or not leave their bed,” explained Halaris. Treatment may require a combination of antidepressant and antipsychotic medications. A review of 10 studies concluded that it may be best to start with an antidepressant drug alone and then add an antipsychotic drug if needed. Another review, however, found the combination of medications was more effective than either drug alone in treating psychotic depression.
If your periods of extreme lows are followed by periods of extreme highs, you could have bipolar disorder (sometimes called manic depressive disorder because symptoms can alternate between mania and depression).
Symptoms of mania include high energy, excitement, racing thoughts, and poor judgment. “Symptoms may cycle between depression and mania a few times per year or much more rapidly,” Halaris said. “This disorder affects about 2 to 3 percent of the population and has one of the highest risks for suicide.” Bipolar disorder has four basic subtypes: bipolar I (characterized by at least one manic episode); bipolar II (characterized by hypomanic episodes — which are milder — along with depression); cyclothymic disorder; and other specified bipolar and related disorder.
People with bipolar disorder are typically treated with drugs called mood stabilizers.
Premenstrual dysphoric disorder, or PMDD, is a type of depression that affects women during the second half of their menstrual cycles. Symptoms include depression, anxiety, and mood swings. Unlike premenstrual syndrome (PMS), which affects up to 85 percent of women and has milder symptoms, PMDD affects about 5 percent of women and is much more severe.
“PMDD can be severe enough to affect a woman’s relationships and her ability to function normally when symptoms are active,” said Halaris. Treatment may include a combination of depression drugs as well as talk and nutrition therapies.
Also called adjustment disorder, situational depression is triggered by a stressful or life-changing event, such as job loss, the death of a loved one, trauma — even a bad breakup.
Situational depression is about three times more common than major depression, and medications are rarely needed — that’s because it tends to clear up over time once the event has ended. However, that doesn’t mean it should be ignored: Symptoms of situational depression may include excessive sadness, worry, or nervousness, and if they don’t go away, they may become warning signs of major depression.
22 Monday May 2023
Posted in Music
≈ Comments Off on Top Songs I listened to in 2022: Thagyan | Zain Zohaib x Quratulain Balouch
20 Saturday May 2023
Posted in Friends
≈ Comments Off on Blue Star Families and Museums
Tags
Blue Star Museums is a partnership between the National Endowment for the Arts and Blue Star Families, in collaboration with the Department of Defense and museums across America, offering free admission to the nation’s active-duty military personnel and their families, including National Guard and Reserve. The 2023 Blue Star Museums program begins on Armed Forces Day, Saturday, May 20, 2023 and ends on Labor Day, Monday, September 4, 2023.
https://www.arts.gov/initiatives/blue-star-museums

19 Friday May 2023
Posted in art
≈ Comments Off on Watch “”Editing is like sculpting in time.” | Artist Fiona Tan | Louisiana Channel
17 Wednesday May 2023
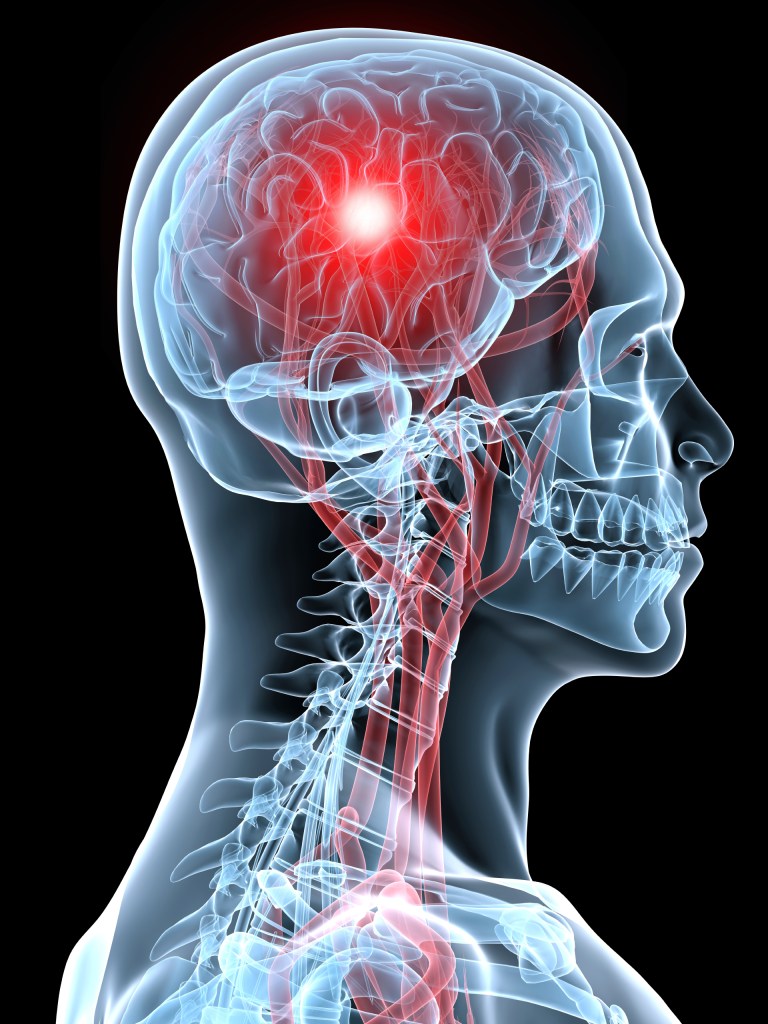
The human brain is the most complex organ in the body. This three-pound mass of gray and white matter sits at the center of all human activity—you need it to drive a car, to enjoy a meal, to breathe, to create an artistic masterpiece, and to enjoy everyday activities. In brief, the brain regulates your body’s basic functions; enables you to interpret and respond to everything you experience; and shapes your thoughts, emotions, and behavior.
The brain is made up of many parts that all work together as a team. Different parts of the brain are responsible for coordinating and performing specific functions. Drugs can alter important brain areas that are necessary for life-sustaining functions and can drive the compulsive drug abuse that marks addiction. Brain areas affected by drug abuse include:
How do the parts of the brain communicate?
The brain is a communications center consisting of billions of neurons, or nerve cells. Networks of neurons pass messages back and forth among different structures within the brain, the spinal cord, and nerves in the rest of the body (the peripheral nervous system). These nerve networks coordinate and regulate everything we feel, think, and do.

To send a message, a brain cell (neuron) releases a chemical (neurotransmitter) into the space (synapse) between it and the next cell. The neurotransmitter crosses the synapse and attaches to proteins (receptors) on the receiving brain cell. This causes changes in the receiving cell—the message is delivered.
How do drugs work in the brain?
Drugs are chemicals that affect the brain by tapping into its communication system and interfering with the way neurons normally send, receive, and process information. Some drugs, such as marijuana and heroin, can activate neurons because their chemical structure mimics that of a natural neurotransmitter. This similarity in structure “fools” receptors and allows the drugs to attach onto and activate the neurons. Although these drugs mimic the brain’s own chemicals, they don’t activate neurons in the same way as a natural neurotransmitter, and they lead to abnormal messages being transmitted through the network.
Other drugs, such as amphetamine or cocaine, can cause the neurons to release abnormally large amounts of natural neurotransmitters or prevent the normal recycling of these brain chemicals. This disruption produces a greatly amplified message, ultimately disrupting communication channels.
How do drugs work in the brain to produce pleasure?
Most drugs of abuse directly or indirectly target the brain’s reward system by flooding the circuit with dopamine. Dopamine is a neurotransmitter present in regions of the brain that regulate movement, emotion, motivation, and feelings of pleasure. When activated at normal levels, this system rewards our natural behaviors. Overstimulating the system with drugs, however, produces euphoric effects, which strongly reinforce the behavior of drug use—teaching the user to repeat it.
Most drugs of abuse target the brain’s reward system by flooding it with dopamine.
How does stimulation of the brain’s pleasure circuit teach us to keep taking drugs?
Our brains are wired to ensure that we will repeat life-sustaining activities by associating those activities with pleasure or reward. Whenever this reward circuit is activated, the brain notes that something important is happening that needs to be remembered, and teaches us to do it again and again without thinking about it. Because drugs of abuse stimulate the same circuit, we learn to abuse drugs in the same way.
Why are drugs more addictive than natural rewards?
When some drugs of abuse are taken, they can release 2 to 10 times the amount of dopamine that natural rewards such as eating and sex do. In some cases, this occurs almost immediately (as when drugs are smoked or injected), and the effects can last much longer than those produced by natural rewards. The resulting effects on the brain’s pleasure circuit dwarf those produced by naturally rewarding behaviors. The effect of such a powerful reward strongly motivates people to take drugs again and again. This is why scientists sometimes say that drug abuse is something we learn to do very, very well.
Long-term drug abuse impairs brain functioning.
What happens to your brain if you keep taking drugs?
For the brain, the difference between normal rewards and drug rewards can be described as the difference between someone whispering into your ear and someone shouting into a microphone. Just as we turn down the volume on a radio that is too loud, the brain adjusts to the overwhelming surges in dopamine (and other neurotransmitters) by producing less dopamine or by reducing the number of receptors that can receive signals. As a result, dopamine’s impact on the reward circuit of the brain of someone who abuses drugs can become abnormally low, and that person’s ability to experience any pleasure is reduced.
This is why a person who abuses drugs eventually feels flat, lifeless, and depressed, and is unable to enjoy things that were previously pleasurable. Now, the person needs to keep taking drugs again and again just to try and bring his or her dopamine function back up to normal—which only makes the problem worse, like a vicious cycle. Also, the person will often need to take larger amounts of the drug to produce the familiar dopamine high—an effect known as tolerance.
Decreased Dopamine Transporters in a Methamphetamine Abuser

How does long-term drug taking affect brain circuits?
We know that the same sort of mechanisms involved in the development of tolerance can eventually lead to profound changes in neurons and brain circuits, with the potential to severely compromise the long-term health of the brain. For example, glutamate is another neurotransmitter that influences the reward circuit and the ability to learn. When the optimal concentration of glutamate is altered by drug abuse, the brain attempts to compensate for this change, which can cause impairment in cognitive function. Similarly, long-term drug abuse can trigger adaptations in habit or non-conscious memory systems. Conditioning is one example of this type of learning, in which cues in a person’s daily routine or environment become associated with the drug experience and can trigger uncontrollable cravings whenever the person is exposed to these cues, even if the drug itself is not available. This learned “reflex” is extremely durable and can affect a person who once used drugs even after many years of abstinence.
What other brain changes occur with abuse?
Chronic exposure to drugs of abuse disrupts the way critical brain structures interact to control and inhibit behaviors related to drug use. Just as continued abuse may lead to tolerance or the need for higher drug dosages to produce an effect, it may also lead to addiction, which can drive a user to seek out and take drugs compulsively. Drug addiction erodes a person’s self-control and ability to make sound decisions, while producing intense impulses to take drugs.
15 Monday May 2023
Posted in Music
≈ Comments Off on Top Songs I listened to in 2022: Go | Abdullah Siddiqui x Atif Aslam
12 Friday May 2023
Posted in Health and wellness, Over 65
≈ Comments Off on Watch “A Multidisciplinary Panel Discussion of Peripheral Artery Disease (PAD)” from Cleveland Clinic.
10 Wednesday May 2023
Posted in Coping Skills, Depression
≈ Comments Off on How to Help Yourself if You Are Depressed
Tags
Depressive disorders can make one feel exhausted, worthless, helpless, and hopeless. It is important to realize that these negative views are part of the depression and do not accurately reflect the actual circumstances. Negative thinking fades as treatment begins to take effect. In the meantime:
09 Tuesday May 2023
Posted in creative arts therapy
≈ Comments Off on Child Life Services Make Treatment Less Scary for Girl With Crohn’s Disease. Cleveland Clinic
08 Monday May 2023
Posted in Music
≈ Comments Off on Top Songs I listened to in 2022: L’Enfer de Stromae en live dans “Boomerang” – Carte blanche
05 Friday May 2023
Posted in Music
≈ Comments Off on Watch “Pulse by Shani Diluka – hypnotic minimalist music by Adams, Riley, Glass, Cage, Monk & more”
Tags